#2020Trends: The Ever-Growing MA Market
Last week’s post in my new series on key trends in healthcare for 2020 focused on innovations in care models that are supporting the rising expectations of members and patients around quality, value and well care. This week, we’re shifting to the next trend in healthcare that is likely to make a big impact on the direction of the industry this year and beyond: the continuing expansion of the Medicare Advantage (MA) market.
As the healthcare industry shifts towards value-based care, MA plans are proving to be a critical stepping stone to simultaneously improving quality of care, cutting down costs and advancing innovation in value-based care models. For example, CMS has expanded MA plans in 2020 to include “non-primary-health-related” benefits like meal delivery, transportation for non-medical needs and in-home services.
Under traditional Medicare, beneficiaries (Seniors at the age of 65+) can go to any hospital or physician and Centers for Medicare and Medicaid Services (CMS) makes reimbursements on a fee-for-service basis. By contrast, Medicare Advantage plans offer benefits to plan enrollees (Seniors at the age of 65+) through private health insurance companies in a fully capitated model. CMS pays these plans a fixed monthly amount for each beneficiary and the plan assumes full financial responsibility for providing all Medicare benefits, and much more.
The good news is that this public-private partnership has consistently delivered better quality of care at a lower cost. According to a recent analysis from the Henry J Kaiser foundation, patients who switched from traditional Medicare to MA plans between 2015 and 2016 had 13.6% less spending than patients who remained in traditional Medicare. Furthermore, other studies have found that risk-adjusted mortality is lower in MA plans vs. traditional Medicare (2.9% vs. 4.3%), which may reflect better care co-ordination and quality of care for patients in MA plans.
A Growing Opportunity
The success of MA plans has made it a popular choice among medicare eligible. In fact, enrollment in MA plans has nearly doubled in the last decade and 34% of Medicare beneficiaries in 2019—22 million people—chose MA Plans over traditional Medicare. Looking ahead, this market will continue to grow at a much faster pace and according to the Congressional Budget Office (CBO) the number of beneficiaries enrolled in MA plans will reach about 47% by the year 2029.
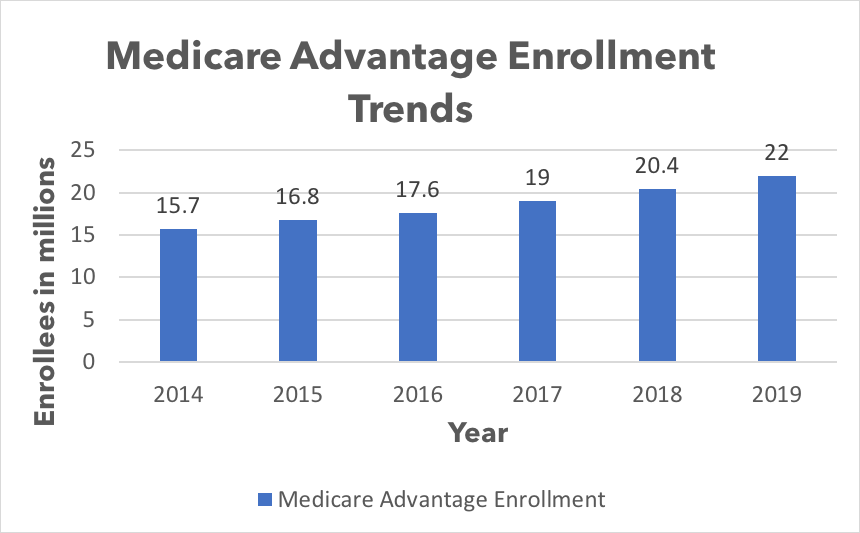
The growth can be explained by several factors, including growth in the aging baby boomer population, (rare) bi-partisan support and comparably favorable margins for payors. As this market continues to expand, we’re starting to see the same kind of pressures and innovations happening across the broader industry.
Factoring in Social Determinants of Health
Last Spring, CMS announced that MA plans will be allowed to begin offering enrollees supplemental, “non-primary health-related” benefits for eligible chronically ill patients with unmet social needs. Plans with these additional benefits are beginning to hit the market. For example, Alignment Healthcare is rolling out new options that include “Grandkids on-demand,” monthly grocery allowances and free transportation to doctor’s appointments via Uber and Lyft. These and other similar benefits designed to address social determinants of health could play a big role in managing the health of chronically ill seniors and lowering long-term utilization costs moving forward.
Senior-Centered Primary Care Services
As the market for MA models has expanded, so too have senior-centered primary care services designed to improve quality of care, increase access and lower utilization costs. Providers like ChenMed, Iora Health and CareMore Health are successfully managing high-risk, senior patients with chronic conditions with new, full-risk clinical models that offer intensive care-coordination and personalization. The tremendous growth of these organizations is likely to encourage additional players to enter the market with similar models.
Medicare Advantage for All?
There is broad, bi-partisan support for shifting federal reimbursement away from fee-for-service towards value-based payment models with risk-based contracts that hold the private sector accountable in delivering better quality and outcomes at a lower cost. MA plans seem to be a good vehicle to be able to do that. As enrollment in MA plans grew to nearly twice its size over the last decade, this coverage model has become an increasingly familiar and popular choice. With several leading candidates calling for “Medicare for All” as part of their presidential campaign platform, I expect we’ll begin to see a pivot to a less controversial universal coverage plan more akin to “Medicare Advantage for All” as the election nears and remaining candidates look for options with more middle-ground appeal.
Regardless of whether it become the model for universal health care in the US, there is no doubt that the Medicare Advantage market will continue to grow and expand in the coming decade.
Coming up Next…
Check back in next week to find out more about the next trend I expect to have a big impact on healthcare in 2020. If you’re not a fan of waiting, feel free to download my full webinar on 2020 Healthcare Trends and get the full scoop right now.





